Is Overpronation
Normally, when you walk or run, your heel is the first part of your foot to strike the ground. As your body weight shifts to the middle of the foot, the arch of the foot naturally flattens out a bit. This flattening is called pronation. If your feet flatten more than normal, it?s called over-pronation or flat feet. Over-pronation can cause many problems, such as an Achilles tendon injury or heel pain. It may lead to knee problems.

Causes
There has been some speculation as to whether arch height has an effect on pronation. After conducting a study at the Rose-Hulman Institute of Technology, Maggie Boozer suggests that people with higher arches tend to pronate to a greater degree. However, the generally accepted view by professionals is that the most pronation is present in those with lower arch heights. To complicate matters, one study done by Hylton Menz at the University of Western Sydney-Macarthur suggests that the methods for measuring arch height and determining whether someone is ?flat-footed? or ?high-arched? are unreliable. He says, ?For this reason, studies investigating the relationship between static arch height motion of the rearfoot have consistently found that such a classification system is a poor predictor of dynamic rearfoot function.
Symptoms
Overpronation can lead to injuries and pain in the foot, ankle, knee, or hip. Overpronation puts extra stress on all the bones in the feet. The repeated stress on the knees, shins, thighs, and pelvis puts additional stress on the muscles, tendons, and ligaments of the lower leg. This can put the knee, hip, and back out of alignment, and it can become very painful.
Diagnosis
When sitting, an over-pronating foot appears quite normal, i.e. showing a normal arch with room under the underside of the foot. The moment you get up and put weight on your feet the situation changes: the arches lower and the ankle slightly turns inwards. When you walk or run more weight is placed on the feet compared to standing and over-pronation will become more evident. When walking barefoot on tiles or timber floors over-pronation is more visible, compared to walking on carpet or grass.
Non Surgical Treatment
The following exercises help retrain the foot and ankle complex to correct overpronation. Step Up and Over. This exercise is designed to integrate skills learned in the Duck Stand, Big Toe Pushdowns and Side Step with Opposite Reach exercises to mimic walking and even running. Using the gluteal muscles and big toe in tandem will prevent overpronation while moving back and forth over the BT in a more effective, balanced motion. Movement Directions. Stand with left foot on top of the BT dome. (Note: For added balance, the right foot can tap on the ground, if needed). Extend right foot backwards to the ground and drop hips into a lunge position. Make sure that the right arm rotates across the left leg (this will activate the gluteal muscles on the left side). Now, step through and over the BT into a front lunge with the right leg forward. While lunging forward, the torso and left arm now rotate over the right leg. Throughout the exercise, push big toe down into the BT. Perform 8 to 10 repetitions on both sides.
Prevention
Many of the prevention methods for overpronation-orthotics, for example-can be used interchangeably with treatment methods. If the overpronation is severe, you should seek medical attention from a podiatrist who can cast you for custom-made orthotics. Custom-made orthotics are more expensive, but they last longer and provide support, stability, and balance for the entire foot. You can also talk with a shoe specialist about running shoes that offer extra medial support and firm heel counters. Proper shoes can improve symptoms quickly and prevent them from recurring. Surgery can sometimes help cure and prevent this problem if you suffer from inherited or acquired pes planus deformity. Surgery typically involves stabilizing the bones to improve the foot?s support and function.
Can I Address Severs Disease In The Home?
Sever?s disease, also known as calcaneal apophysitis or Osgood-Schlatter syndrome of the foot. This traction apophysitis is secondary to repetitive microtraumata or overuse of the heel in young athletes. The calcaneus is situated at the most plantar posterior aspect of the foot. The Achilles tendon inserts to the lower, posterior and slightly medial aspect of the calcaneus. The plantar fascia originates from the medial tubercle on the plantar aspect of the calcaneus. Proximal to the epiphysis is the apophysis, where the Achilles tendon actually inserts. The calcaneal growth plate and apophysis are situated in an area subject to high stress from the plantar and Achilles tendon.
Causes
Sever?s disease is often an overuse injury. It can be caused by playing sports, especially those involving high impact. Sever?s disease can also be linked to growth which can place a stress on the attachment of the Achilles tendon.
Symptoms
The most common symptom of Sever's disease is acute pain felt in the heel when a child engages in physical activity such as walking, jumping or running. Children who are very active athletes are among the group most susceptible to experiencing Sever's disease because of the extreme stress and tension they place on their growing feet. Improper pronation, the rolling movement of the foot during walking or running, and obesity are all additional conditions linked to causing Sever's disease.
Diagnosis
The doctor may order an x-ray because x-rays can confirm how mature the growth center is and if there are other sources of heel pain, such as a stress fracture or bone cyst. However, x-rays are not necessary to diagnose Sever?s disease, and it is not possible to make the diagnosis based on the x-ray alone.
Non Surgical Treatment
In general, the goals for treatment include reducing the localized areas of inflammation. We recommend that patients utilize Ibuprofen every six to eight hours as needed. Stretching exercises on a daily basis, as well as prior to activity is thought to be helpful as well. Following work-outs and increased activities, it may be helpful to apply ice over affected areas. Heel cups are also available to provide cushion in shoes. In addition, for more severe symptoms, it may be helpful to refrain from sports and/or immobilize the area for a few weeks to help reduce the inflammation.
Exercise
For children with Sever's disease, it is important to habitually perform exercises to stretch the hamstrings, calf muscles, and the tendons on the back of the leg. Stretching should be performed 2-3 times a day. Each stretch should be performed for 20 seconds, and both legs should be stretched, even if the pain is only in one heel. Heel cups or an inner shoe heel lifts are often recommended for patient suffering from Sever's disease. Wearing running shoes with built in heel cups can also decrease the symptoms because they can help soften the impact on the heel when walking, running, or standing.
What Is Adult Aquired Flat Foot ?
Overview
PTTD is a common condition treated by foot and ankle specialists. Although there is a role for surgical treatment of PTTD, conservative care often can prevent or delay surgical intervention. Decreasing inflammation and stabilizing the affected joints associated with the posterior tibial tendon can decrease pain and increase functional levels. With many different modalities available, aggressive nonoperative methods should be considered in the treatment of PTTD, including early immobilization, the use of long-term bracing, physical therapy, and anti-inflammatory medications. If these methods fail, proper evaluation and work-up for surgical intervention should be employed. 
Causes
Many health conditions can create a painful flatfoot, an injury to the ligaments in the foot can cause the joints to fall out of alignment. The ligaments support the bones and prevent them from moving. If the ligaments are torn, the foot will become flat and painful. This more commonly occurs in the middle of the foot (Lisfranc injury), but can also occur in the back of the foot. In addition to ligament injuries, fractures and dislocations of the bones in the midfoot can also lead to a flatfoot deformity.
Symptoms
Patients will usually describe their initial symptoms as "ankle pain", as the PT Tendon becomes painful around the inside of the ankle joint. The pain will become more intense as the foot flattens out, due to the continued stretching and tearing of the PT Tendon. As the arches continue to fall, and pronation increases, the heel bone (Calcaneus) tilts into a position where it pinches against the ankle bone (Fibula), causing pain on both the inside and outside of the ankle. As the foot spends increased time in a flattened, or deformed position, Arthritis can begin to affect the joints of the foot, causing additional pain.
Diagnosis
Observe forefoot to hindfoot alignment. Do this with the patient sitting and the heel in neutral, and also with the patient standing. I like to put blocks under the forefoot with the heel in neutral to see how much forefoot correction is necessary to help hold the hindfoot position. One last note is to check all joints for stiffness. In cases of prolonged PTTD or coalition, rigid deformity is present and one must carefully check the joints of the midfoot and hindfoot for stiffness and arthritis in the surgical pre-planning.
Non surgical Treatment
Treating PTTD is almost always easier the earlier you catch it. So, the first step in treatment is to see your doctor as soon as you begin experiencing painful symptoms. However, once your condition has been diagnosed, your podiatrist will likely try to give the upset tendon a bit of a break so it?ll calm down and stop being so painful. This can often be accomplished by immobilizing the foot using tape and padding, braces, or casts, depending on what your podiatrist believes will work best for you, and depending on the severity of your condition. You may also be instructed to reduce inflammation by applying ice to the area (usually 40 minutes on and 20 minutes off, with a thin towel between you and the ice). Or, you might take anti-inflammatory medications like ibuprofen (steroidal anti-inflammatory meds are actually likely to make this problem worse, and are not usually recommended in treating PTTD), or use ultrasound therapy. Once the inflammation has gone down a bit, your podiatrist may recommend using orthotics (prescription shoe inserts) to support your damaged arch. Ankle braces can also be helpful. 
Surgical Treatment
In cases of PTTD that have progressed substantially or have failed to improve with non-surgical treatment, surgery may be required. For some advanced cases, surgery may be the only option. Surgical treatment may include repairing the tendon, tendon transfers, realigning the bones of the foot, joint fusions, or both. Dr. Piccarelli will determine the best approach for your specific case. A variety of surgical techniques is available to correct flexible flatfoot. Your case may require one procedure or a combination of procedures. All of these surgical techniques are aimed at relieving the symptoms and improving foot function. Among these procedures are tendon transfers or tendon lengthening procedures, realignment of one or more bones, or insertion of implant devices. Whether you have flexible flatfoot or PTTD, to select the procedure or combination of procedures for your particular case, Dr. Piccarelli will take into consideration the extent of your deformity based on the x-ray findings, your age, your activity level, and other factors. The length of the recovery period will vary, depending on the procedure or procedures performed.
Foot Arches Pain Running
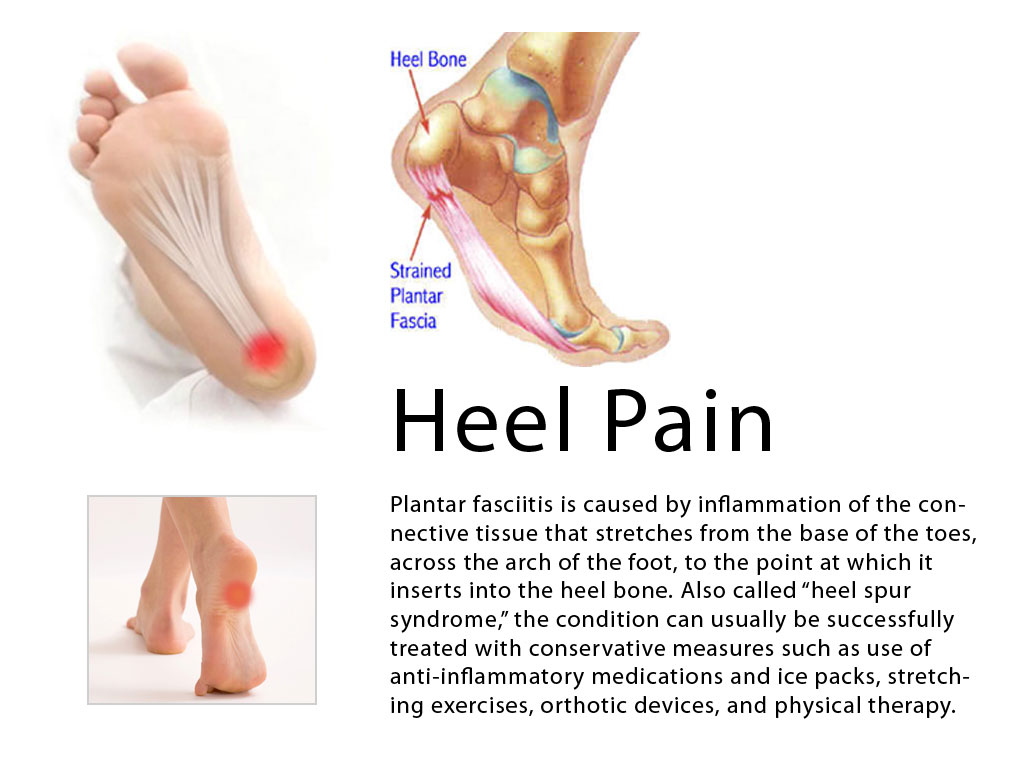
The plantar fascia is a sturdy structure but the degree of stress that it takes makes it susceptible to injury. A force equal to almost three times body weight passes through the foot with each step. On running, this typically happens about 90 times a minute. Plantar fasciitis is thought to be a traction and overuse injury. Damage to the plantar fascia is usually in the form of micro-tears. It is a degenerative rather than an inflammatory process. Damage tends to occur near the heel, where stress on the fibres is greatest, and where the fascia is the thinnest. The fascia broadens as it extends toward the toes.
Plantar fasciitis is often associated with calcaneal spurs. These are depositions of calcium where the fascia suffers most damage. Spurs are most commonly on the medial side at the origin of the fascia from the calcaneum. Spurs are the result of the process of plantar fasciitis and not the cause of the pain. It can present bilaterally.

Causes
Sprains, strains, bruises, and fractures may be the result of a single stress or a combination of stresses to the foot. A blunt-force injury such as someone stepping on your foot may result not only in a bruise (contusion), but also in damage to the primary and secondary structures of the foot. Many of the muscles of the lower leg and foot attach on or near the arch. Injured or tight muscles may lead to incorrect biomechanics and in turn cause arch pain. Injury to the bones of the foot can be caused by a single blow or twist to the arch or also by repetitive trauma, which can result in a stress fracture. A sprain of the arch occurs when the ligaments which hold the bones together are overstretched and the fibers tear. The muscles of the foot may be strained by overstretching, overuse, overloading, bruising, or being cut by stepping on a sharp object. Arthritis of the arch joints may also occur if the foot is subjected to repetitive movements that stress the arch.
Symptoms
The majority of children and adults with flexible flatfeet never have symptoms. However, their toes may tend to point outward as they walk, a condition called out-toeing. A person who develops symptoms usually complains of tired, aching feet, especially after prolonged standing or walking. Symptoms of rigid flatfoot vary depending on the cause of the foot problem.
Diagnosis
In a person of any age, the doctor will ask about occupational and recreational activities, previous foot trauma or foot surgery and the type of shoes worn. The doctor will examine your shoes to check for signs of excessive wear. Worn shoes often provide valuable clues to gait problems and poor bone alignment. The doctor will ask you to walk barefoot to evaluate the arches of the feet, to check for out-toeing and to look for other signs of poor foot mechanics.
Non Surgical Treatment
If it is flat feet, then you'd seek professional advice and maybe need orthotics, or arch supports to prevent the pressures and to stop the pain. One of the other reasons you can get pain in this area of the foot is plantar fasciitis. The plantar fascia is a membrane that is inside of the skin and attaches to the heel bone here. It divides into three bands that go out of the foot here: the outer band, the central band, and the medial band here. Often, from impact, you get an inflammation of that attachment to the heel bone and this can often spread up the medial band and this is another way of getting pain in that arch. Now, the way to treat that is also using arch supports but also heel cushions, better soled shoes to prevent the pressure. These things normally disappear after a year, 18 months. Plantar fasciitis is easier to treat because it's not a long term problem. If you do need arch support, something like this would be very good for both problems.

Surgical Treatment
In rare cases, surgery may be needed if a child has flat feet caused by a problem they're born with (a congenital abnormality). The foot may need to be straightened or the bones may need to be separated if they're fused together. Painkillers and insoles are the first treatment options for flat feet that are caused by a joint problem, such as arthritis or a torn tendon. However, surgery may be recommended if the injury or condition is severely affecting your feet. Where flat feet are caused by a condition that affects the nervous system, special shoes, insoles, or supportive foot or leg braces may be needed. Again, in severe cases, an operation may be needed to straighten the feet.
Stretching Exercises
Calf Stretching in Bed. As you may already know, the first few steps out of bed in the morning can be the worst of the day. Those first few steps can be enough to reaggravate your condition putting you into a cycle of inflammation and pain. The best way to help break that cycle is to stretch your calf before taking those first steps in the morning. When the muscles in your calf are tight, they pull on the heel bone, making your plantar fascia very taut and prone to injury. To help loosen those muscles, take a towel or belt and loop it around the ball of your foot. Keeping your leg straight, gently pull towards your body until you feel a stretch in the lower part of your leg. Hold that for 30 seconds and repeat up to 5 times before taking your first step out of bed. Plantar Fascia Stretching. Loosening up the tissues that are irritated probably makes sense to you, but you may not know how to do so. Luckily, there?s a very simple way. All you have to do is pull your toes up with your hand until you feel a stretch along the ball of your foot. You may feel the stretch anywhere from the ball of your foot to your heel. Holding this position for 30 seconds a few times can make a world of difference in your pain levels. Calf Stretching. I know, it probably seems like overkill, but stretching out the muscles in the lower leg is an integral step to recovery. There are two main muscles in the lower leg that attach to the heel, so we?ll work on stretching them both out. Stand against a wall and slide one leg back, pushing the heel down towards the floor (first picture). When you feel a stretch in the lower part of your leg, hold it for 30 seconds. After those 30 seconds are up, bend your knees until a deeper stretch is felt a bit lower in the leg (second photo). Again, hold this stretch for 30 seconds and repeat this until you?ve done it 3 times on each leg. Who doesn?t love a good massage? I suppose you could pay for someone to rub out the tissues in the bottom of your foot, but if you?re looking for a cheaper alternative, look no further than the humble tennis ball. Placing a tennis ball on the ground and gently rolling it under foot for a few minutes can help loosen up your plantar fascia, making it much less likely to become irritated. Put enough pressure on the ball to get a deep massage. You may feel some soreness, but back off if you feel any pain.Tennis Ball Massage While using the tennis ball is great for keeping things loose, sometimes it?s worth doing some icing at the same time for some inflammation control. Freezing a water bottle and rolling it under your foot for 10 minutes at the end of the day can be a very effective way to keep inflammation in check while staying loose. It might not be the most comfortable thing in the world, but ?Brrr? is better than ?Ouch? any day. One thing to keep in mind is that while these tips have been proven to work, they?re not an instant fix. It can take a few weeks of consistency with them before your pain levels begin to change. If you?re not seeing any improvement after making an honest effort, it may be time to look into some different treatment methods with your doctor such as formal PT, orthotics, a weight-loss plan, or others.